*No quick fix for an ailing health system
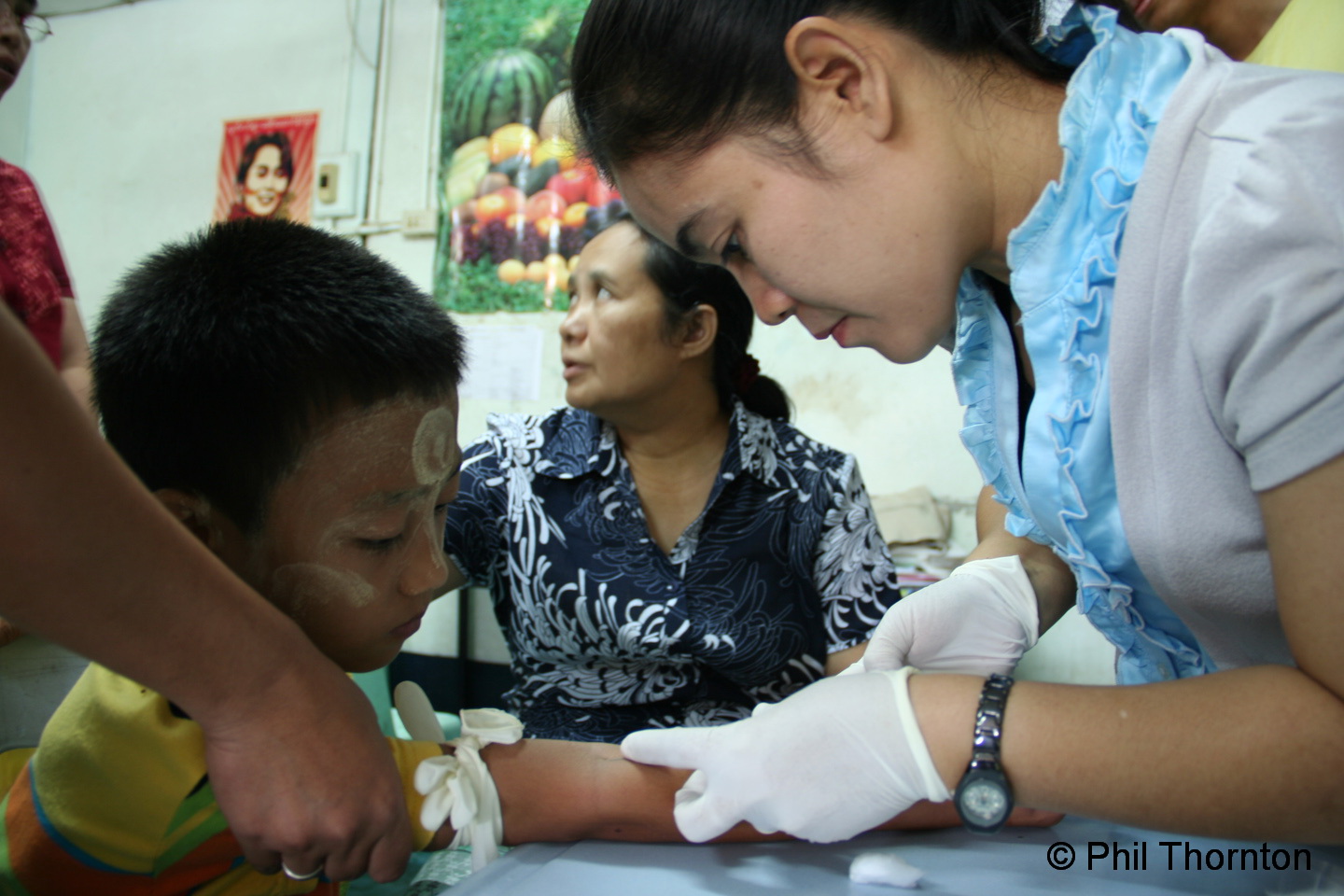
Ethnic communities have spent decades building vital services in the absence of government help, but there are now fears interference could result in their work being undermined.
While acknowledging Myanmar needs help, Cynthia Maung is not optimistic that a $100 million (about 3.2 billion baht) agreement with the World Bank for essential health services will benefit ethnic community health organisations or their patients.
Dr Cynthia stops taking notes on a large pad, removes her glasses and explains that during decades of armed conflict, ethnic people working under dire circumstances still managed to build a functioning health system.
“We have spent more than 20 years building and strengthening the capacity of ethnic workers to provide essential community health services,” she said. “We have built up expertise that is internationally recognised and we have a proven health system in place that works, but desperately needs resources to address the chronic health crisis in the region.
“Working with the ethnic communities, we trained more than 2,600 health workers, operate 114 clinics, resource 125 mobile and backpack teams, and have developed a structure that delivers health care to a target population of around 500,000 people.”
Dr Cynthia’s decades of health work in eastern Myanmar have not gone unnoticed by humanitarian organisations and international and regional governments who have given her a staggering number of awards.
She believes the Myanmar government’s current centralised health system is broken and for reforms to work incoming resources have to be shared with ethnic community health providers.
Dr Cynthia is the founder of the Mae Tao Clinic in the Thai border town of Mae Sot. The clinic, also known as Dr Cynthia’s Clinic, saw about 140,000 people from Myanmar last year. The small lane that joins the clinic’s various health departments is testimony that all is not well with Myanmar’s health system. A constant stream of mini-buses and cars with Yangon number plates disgorge and pick up patients who are unable to access health care in Myanmar.
A BROKEN SYSTEM
After a series of oppressive military regimes, 60 years of civil war and pitiful government investment, Myanmar’s health system became so neglected and corrupt that in 2000 the World Health Organisation ranked it second-last out of 191 countries assessed.
“We have two parallel health systems now in Burma, one is implemented by the government and the other is implemented by ethnic community health organisations,” Dr Cynthia said. “What is needed is convergence and not for the ethnic health system to be swept away by a centralised system out of touch with community needs.”
On Thursday a report, The Long Road to Recovery, was released highlighting the plight of health care in Myanmar. The report is the result of surveys conducted in remote and displaced communities in eastern Myanmar by a network of organisations called the Health Information System Working Group (HISWG).
The University of California, Los Angeles and Harvard helped the community-based group design the survey and analyse the data. The survey covered 6,620 households in 64 townships, and “had a target population of 456,786 people”.
It was the first such survey since the government and the Karen signed a ceasefire agreement in 2012.
WORKING FOR THE PEOPLE
Saw Nay Htoo, a Burma Medical Association director and member of the HISWG network, has spent 17 of his 42 years as a medic working for displaced communities in eastern Myanmar.
Saw Nay Htoo has a degree in biomedical science from Mahidol University. He said the ethnic health system had progressed from being a basic reactive service to one capable of carrying out large-scale population surveys that can help plan effective health strategies.
“When I first started in 1991 we could only provide a basic service. Remember, we were also regarded as illegal and we ran the risk of being jailed or more likely killed by the government’s military,” he said.
“Now we can plan our health system needs based on demographics, migration, mortality, reproductive health, child health, sanitation, food access, nutrition and access to health services.”
Saw Nay Htoo is concerned that the huge amounts of international money promised for Myanmar health services will instead be used by the government to bolster its control over ethnic territory.
“Funding for health is getting complicated. International non-government organisations who do not understand, or just ignore, the country’s fragile political situation or the health services we have already put in place, have made it even more complex.”
Saw Nay Htoo said international NGOs, in their rush to ingratiate themselves with the government, ignored the years of hard slog ethnic health workers had endured to establish community health services.
“They don’t see us. Instead of working with us and using the health data that we have been collecting and analysing for years to plan programmes, they want and are prepared to work only with the government. It is stupid to ignore our research — they need to work with both sides as equal partners.”
Saw Nay Htoo said bypassing ethnic health service providers risked adding to the layers of mistrust that already exist between the central government and ethnic people.
“It is crucial that NGOs acknowledge and recognise the ethnic health systems and structures if they really want to see Burma develop. NGOs should be aware that they are a short-term solution — we know they will eventually leave.”
In detailing the difficulties, The Long Road to Recovery survey found that malaria was the “primary reported cause of death across all age groups and the second main cause of death among children under five”.
“For the vast majority of people in eastern Burma official Burmese government health facilities remain unavailable or inaccessible,” the report found.
It added: “Where government services are available, patients must pay out-of-pocket for almost all government health services including medication, medical supplies and diagnostic tests.”
The report also said patients had to cover the cost of food, cleaning and “are often asked to make ‘donations’ to the staff”.
WE MAKE DO
Saw Nay Htoo sweeps his arm around his large office that also serves as a staff eating area, packing room for medicines, storage and meeting room. From there, he is often astonished at reports in the regional media of the huge amounts UN departments and international NGOs spend renting offices in Myanmar.
“We do not require the sort of building they say they need to work in Burma. We’d rather use the money for the community, for us a simple office will do.”
The rent for the Burma Medical Association’s large, two-storey concrete residential house and garden on the edges of the Thai-Myanmar border costs 11,000 baht a month, or about $330.
The United Nations Children Fund (Unicef) attracted international media attention and scorn when it was reported that it paid a monthly rent of $87,000 to a former military official.
Saw Nay Htoo is incredulous when he starts to do the maths.
“That’s more than a $1 million a year! Our entire Back Pack Health Workers Team of 1,450, who treat around 44,000 cases and deliver primary health services to a target population of 200,000, work for less than what Unicef paid in office rent for a year.”
Saw Nay Htoo underlines the paltry amounts that ethnic health workers spend when he explains that the Back Pack team members earn about 1,000 baht a month — $32.
RECOGNITION LONG OVERDUE
Vit Suwanvanichkij from the Johns Hopkins Centre for Public Health and Human Rights agreed that the work ethnic services do has to be recognised.
“If we are to have any hope of adequately and appropriately addressing these health priorities, ethnic health providers must be included as equal partners in public health initiatives affecting their communities.”
Dr Vit said recognition for ethnic health services would also be critical at a time when Myanmar moves towards reconciliation.
“This would not only recognise their efforts and the strides they have made in addressing these and other pressing health issues, it would also strengthen their work during this critical transition period, helping to maintain and build upon the progress they have made already, but also … helping to bring about greater ethnic trust and national reconciliation.”
Dr Vit acknowledged that in Myanmar, with a government notorious for reneging on political promises, the opposite can also be true.
“Failing to recognise ethnic health organisations and their work risks further marginalising ethnic communities, heightening ethnic mistrust which is already high as a result of past and ongoing abuses by the central authorities. Solely supporting centralised, top-down initiatives risks fuelling this, imperilling access to health care and, ultimately, the prospects of ethnic reconciliation and true peace.”
In her foreword to The Long Road to Recovery, Dr Cynthia warned that development and aid projects could have had a negative impact on health.
“Many people have been forced to relocate or had their land confiscated to make way for development projects. While humanitarian aid can be an important tool to help populations in need, it can also have negative consequences if it is implemented in a way that is not sensitive to the needs of the people it is designed to help.”
*This article first appeared on Bangkok Post on 22 February 2015.




